Pneumococcal Disease
Pneumococcal disease (PD) is a common infection. It is caused by a bacterium called Streptococcus pneumoniae, also known known as pneumococcus
Pneumococcal disease (PD) is a common infection. It is caused by a bacterium called Streptococcus pneumoniae, also known known as pneumococcus. There are instances in which pneumococcal disease causes serious health problems or is life-threatening, especially in the elderly, small children, and people with weakened immune systems. Regular vaccinations can prevent pneumococcal disease and disease complications.
Symptoms
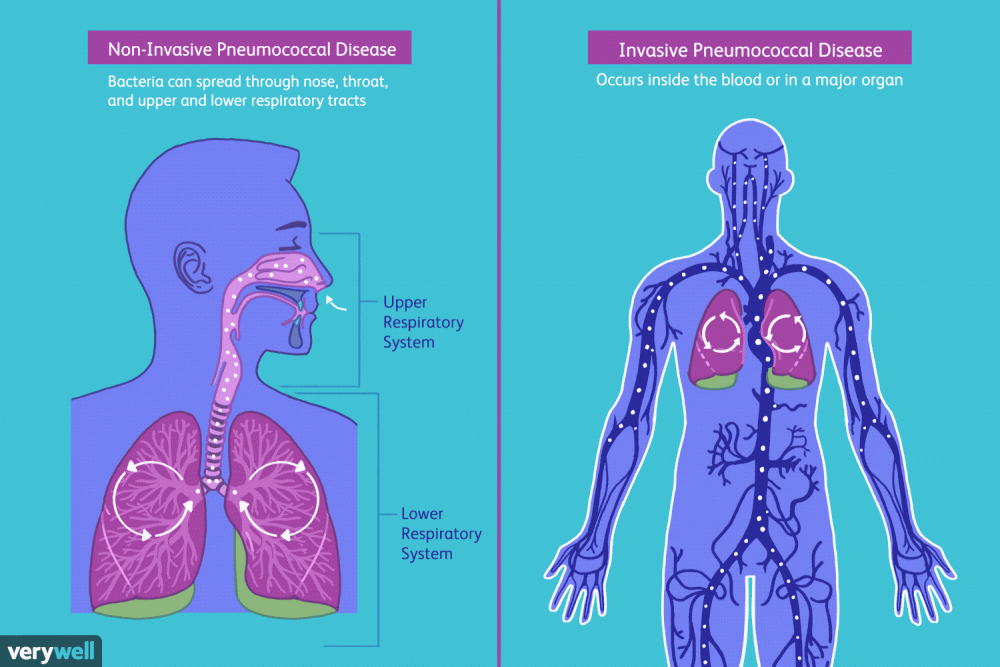
There are two main types of pneumococcal disease: non-invasive and invasive. The non-invasive form of the disease is less serious, whereas invasive is fatal in 10% of cases according to the Centers for Disease Control and Prevention (CDC).
Non-Invasive Pneumococcal Disease
Non-invasive pneumococcal disease causes a mild infection where the s. pneumoniae bacteria can spread through the nose, throat, and upper and lower respiratory tracts. The bacteria is associated with a number of conditions.
- Acute bronchitis. Bronchitis is a condition where the airways are inflamed, causing a cough with mucus. It usually lasts two to three weeks and is more common in younger children.
- Sinusitis. This condition is quite common in people of all ages and causes inflammation of the sinuses in the skull and face. Symptoms include pain, swelling, and tenderness in the eyes, cheeks, and forehead.
- Otitis media. This condition causes inflammation in the middle ear. Symptoms include fluid in the ear, swelling, and earache. If there is perforation of the eardrum, there may be pus drainage to the ear canal. Children who develop otitis media may end up with repeated ear infections and/or may need ear tubes.
Non-invasive pneumococcal infections are usually mild and rarely result in complications. If severe, however, they can cause hearing loss or brain damage.
Invasive Pneumococcal Disease
Invasive PD is more serious than the non-invasive type and occurs inside the blood or in a major organ. There are several types of invasive pneumococcal disease including pneumonia, meningitis, sepsis, bacteremia, osteomyelitis, and septic arthritis.
- Pneumonia. Pneumonia is a serious infection or one of both lungs. Symptoms include difficulty breathing, chest pain, fever, chills, and cough. Five out of every 100 people who develop pneumonia die from it and the risk of death is highest in elderly people.
Additional complications of pneumonia include empyema, which is an infection of the membrane space around the lungs and chest cavity as well as pericarditis, an infection of the sac around the heart. Pneumonia may also cause lung problems, including blockage of the lung airway (endobronchial obstruction), lung collapse (atelectasis), and abscess (pus collection) in the lungs.
-
- Meningitis. Meningitis causes inflammation of the meninges, the membranes covering the brain and spinal cord. Symptoms include stiffness of the neck, headache, fever, confusion, and light sensitivity. Meningitis is a very severe type of invasive PD. According to the CDC, one in 15 children under age five dies from this infection. The chance of death is also higher in older adults, and the infection can lead to developmental delays in children and hearing loss in both children and adults.
- Sepsis. This is a life-threatening infection. Symptoms include fever, chills, confusion, rapid heartbeat, breathing problems, clammy skin, and pain. Septic shock is a life-threatening complication of sepsis. Septic shock causes an altered mental state, problems with oxygenation and breathing, low blood pressure, rapid heart rate, and low urine output. At least 50% of people who develop septic shock will die.
- Bacteremia. This is a bacterial infection of the blood that may be fatal. It often progresses quickly and causes sepsis. Symptoms include fever, chills, and confusion. About one in 100 children under than age five who develop this infection die and the chance of death is also high in the elderly.
- Osteomyelitis. This disease causes inflammation and infection in a bone. Symptoms include fever, irritability, fatigue, nausea, and tenderness, redness, warmth, swelling, and lost range of motion in the affected bone. Complications include bone poisoning, bone abscesses, and bone death.
- Septic arthritis. This type of arthritis causes infection in a joint. Symptoms include fever and chills, fatigue, weakness, and severe pain, swelling, warmth, redness, and stiffness in the affected joint. Complications include osteoarthritis and osteomyelitis
Causes
Anyone can get pneumococcal disease, but some people have a greater risk than others. People with a heightened risk for PD include:
- anyone under age 2 or older than age 65
- anyone with a weakened immune system
- anyone with a chronic condition such as diabetes, heart disease, kidney disease, or autoimmune disease
- smokers
- people living in long-term care institutions
The s. pneumoniae bacteria is common in the noses and throats of children. It can be spread through droplets in the air, such as when a person sneezes or coughs.
Most people who become exposed to s. pneumoniae have no symptoms because their immune systems fight the germs and keep them from moving to other parts of the body. But in people who have weak immune systems, bacteria moves to the throat, lungs, blood, sinuses, or the brain, eventually leading to a severe infection.
People with weak immune systems include those who:
- have a condition affecting the immune system such as HIV or AIDS
- take medications that suppress the immune system such as with autoimmune diseases or after an organ transplant
- are undergoing medical treatments, including chemotherapy
- contract another infection, such as the flu
Diagnosis
A diagnosis of pneumococcal disease involves assessing symptoms and performing a physical exam. Depending on the severity of symptoms and which body parts are affected, your doctor may recommend additional testing.
Additional tests may include:
- Lab work. Your doctor may want to test sputum (a mix of saliva and mucus coughed up) or fluid from the lungs, joints, bone, heart or an abscess (pocket of pus). A cerebrospinal fluid test (CSF) with a lumbar puncture can help with making a diagnosis of meningitis.
- Chest X-ray. A chest X-ray can reveal a shadow that may indicate a pneumonia infection or fluid in the pleural cavity of a lung, and also it may assist in diagnosing other infections including acute chest or lung infections.
Treatment
Treatment depends on the type of pneumococcal disease. Noninvasive pneumococcal infections may not need treatment. However, your doctor may likely recommend antibiotics to prevent complications.
Invasive pneumococcal infections will require antibiotics. Your doctor will likely prescribe broad-spectrum antibiotics right away even before determining what type of bacteria is involved because waiting may cause serious complications. After testing reveals the type of bacteria, your doctor may give you a target antibiotic to treat the specific bacterium.
Antibiotics are usually given in pill or liquid form by mouth. A serious infection may require a hospital stay and intravenous (IV) antibiotics. If you are having problems breathing, your treatment plan may also include supplemental oxygen.
Prevention
The best prevention of pneumococcal disease is vaccination. The Centers for Disease Control and Prevention recommend routine vaccinations for children, older adults, and anyone age two through 64 years with certain medical conditions.
While there are numerous strains of s. pneumoniae and vaccination cannot prevent all of them, pneumococcal vaccines can protect you from the most common strains. They are safe and effective and side effects tend to be mild and may include swelling and soreness at the injection site, fever, and muscle pain.
Experts believe the benefits of vaccination for PD outweigh the potential risks. You cannot get pneumococcal disease from vaccination.

