Newborns and Mortality Fact Sheet
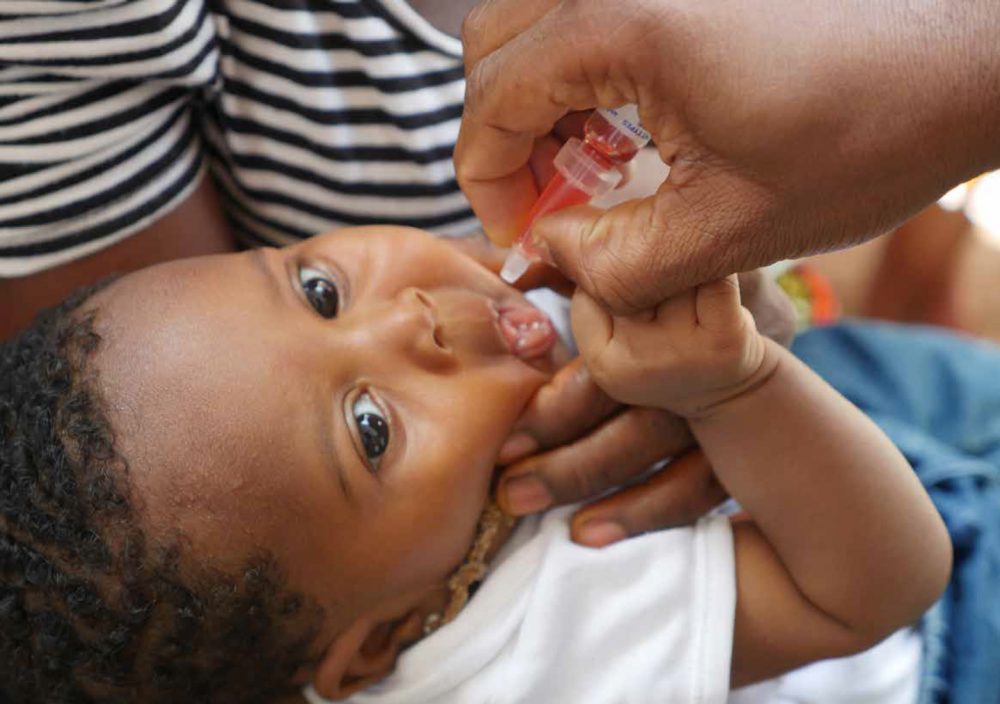
The vast majority of newborn deaths take place in developing countries where access to health care is low.
Fact Sheet
Key facts
- Every year nearly 45% of all under 5 child deaths are among newborn infants, babies in their first 28 days of life or the neonatal period.
- Three quarters of all newborn deaths occur in the first week of life.
- In developing countries nearly half of all mothers and newborns do not receive skilled care during and immediately after birth.
- Up to two thirds of newborn deaths can be prevented if known, effective health measures are provided at birth and during the first week of life
The vast majority of newborn deaths take place in developing countries where access to health care is low. Most of these newborns die at home, without skilled care that could greatly increase their chances for survival.
Skilled health care during pregnancy, childbirth and in the postnatal (immediately following birth) period prevents complications for mother and newborn, and allows for early detection and management of problems. In addition, AHO now recommend home visits by a skilled health worker during a baby’s first week of life to improve newborn survival. Newborns in special circumstances, such as low-birth-weight babies, babies born to HIV-positive mothers, or sick babies, require additional care and should be referred to a hospital.
Causes
Newborn, or neonatal, deaths account for 45% of all deaths among children under 5. The majority of all neonatal deaths (75%) occur during the first week of life, and between 25% to 45% occur within the first 24 hours.
The main causes of newborn deaths are prematurity and low-birth-weight, infections, asphyxia (lack of oxygen at birth) and birth trauma. These causes account for nearly 80% of deaths in this age group.
Prevention strategy: skilled health care at home
Up to two thirds of newborn deaths could be prevented if skilled health workers perform effective health measures at birth and during the first week of life.
Home visits by a skilled health worker immediately after birth is a health strategy that can increase newborn survival rates. The strategy has shown positive results in high mortality settings by reducing newborn deaths and improving key newborn care practices. While home births are very common in developing countries, only 13% of women in these countries receive postnatal care in the first 24 hours. Many mothers who give birth in health facilities cannot return for postnatal care because of financial, social or other barriers. The first days of life are the most critical for newborn survival.
Home care visits should occur on days 1 and 3 of a newborn’s life, and if possible, a third visit should take place before the end of the first week of life (day 7).
Newborns
During home visits, skilled health workers should perform the following measures.
- promote and support early (within the first hour after birth) and exclusive breastfeeding;
- help to keep the newborn warm (promoting skin-to-skin contact between mother and infant);
- promote hygienic umbilical cord and skin care;
- assess the baby for signs of serious health problems, and advise families to seek prompt medical care if necessary (danger signs include feeding problems, or if the newborn has reduced activity, difficult breathing, a fever, fits or convulsions, or feels cold);
- encourage birth registration and timely vaccination according to national schedules;
- identify and support newborns that need additional care (e.g. those that are low-birth-weight, sick or have an HIV-infected mother); and
- if feasible, provide home treatment for local infections and some feeding problems.
Higher risk newborns
Some newborns require additional attention and care during home visits to minimize their health risks.
Low-birth-weight babies:
- increased attention to keeping the newborn warm, including skin-to-skin care immediately following birth for at least an hour, unless there are medically justifiable reasons for delayed contact with the mother;
- assistance with initiation of breastfeeding within the first hour after birth, such as helping the mother express breast milk for feeding the baby from a cup if necessary. (If a baby is unable to accept feeding from a cup, the newborn should be referred to a hospital);
- extra attention to hygiene, especially hand washing;
- extra attention to health danger signs and the need for care; and
- additional support for breastfeeding and monitoring growth.
Sick newborns:
- the families of newborns with severe illness should be helped in locating a hospital or facility to care for the baby; and
- newborns should be treated for infections (e.g. with antibiotic injections) by a nurse, doctor or skilled health worker.
Newborns of HIV-infected mothers:
- preventive antiretroviral treatment (ART) for mothers and newborns to prevent opportunistic infections;
- HIV testing and care for exposed infants; and
- counselling and support to mothers for infant feeding. (Community health workers should be aware of the specialized issues around infant feeding. Many HIV-infected newborns are born prematurely and are more susceptible to infections.)
AHO Action Plan
AHO and its partners agree that a core principle underlying maternal, newborn and child health efforts is lifelong access to health care: a continuum of care for the mother starting from long before pregnancy (during childhood and adolescence) through pregnancy and childbirth. The continuum begins again with adequate newborn care for the new life. As appropriate, care can be delivered in the home and community, as well as health clinics and hospitals.
Budget for AHO Action Plan
US$75 million
Please donate to save children’s lives
Sources: WHO, UNICEF, UN, PAHO, NHS

