
Ethiopia
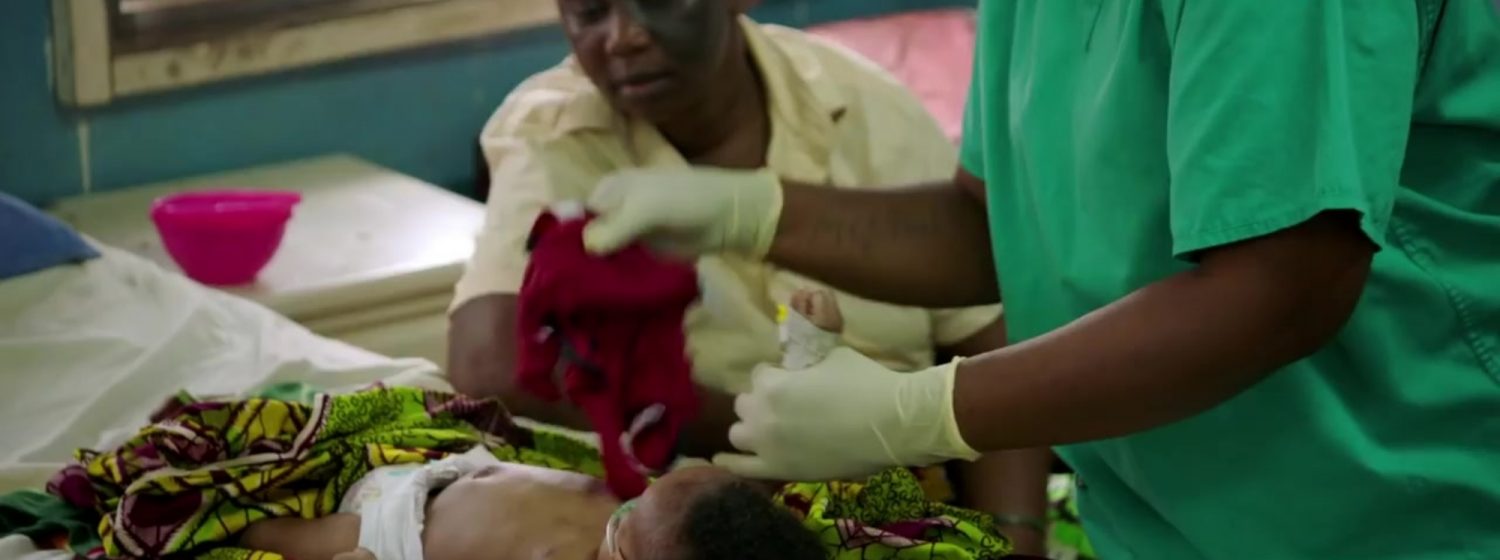
Ethiopia, in the Horn of Africa, is a rugged, landlocked country split by the Great Rift Valley. With archaeological finds dating back more than 3 million years, it’s a place of ancient culture. Its population is 94 million people and GDP per capita of USD 505 (2013).
Ethiopia is Africa’s second most populous country, with 90 million people. In recent years, Ethiopia has made health a priority and has built an ambitious health extension program, with tens of thousands of Health Extension Workers who now form the backbone of the health care system, serving people through the community health posts all over the country. Health extension workers deliver diagnosis, supervise treatment for TB, and facilitate advocacy and community mobilization. Ethiopia is one of the largest implementers of grants supported by the Global Fund, and has achieved significant results, reducing child mortality, expanding HIV prevention, treatment and care, and improving maternal health. However, Ethiopia continues to face serious health challenges. Nearly 800,000 people are estimated to be living with HIV and it is the second leading cause of death in the country. Ethiopia is the ninth-highest TB burden country in the world, is one of the 27 high multidrug-resistant TB burden countries, and annually records nearly 3 million cases of malaria.
AHO PRIORITIES FOR HEALTH DELIVERY PLAN IN ETHIOPIA
- Consolidate the Unified Health System (UHS), strengthening managerial capacity in the three spheres of government and facilitating consensus-building on objectives and results through pacts between UHS managers (bipartite and tripartite), integrated planning and programming activities, and use of the integrated nature of the three levels of care to improve the equity, quality, and efficiency of services, and operationalize prevailing UHS standards.
- Promote the functional integration of databases and information systems that support health decisions and policies, particularly those for epidemiological and managerial surveillance activities and programs, establishing remote electronic access services, the Virtual Health Library (VHL) and the Integrated Health Information Network (RIPSA).
- Develop and implement environmental health and sanitation policies to reduce the disease and mortality burden and improve the health and well-being of the population.
- Strengthen actions and programs to prevent, monitor, and control communicable diseases, particularly vaccine preventable diseases; STD/HIV; tuberculosis; leprosy; vector-borne diseases such as malaria, dengue, yellow fever, and zoonoses, especially, rabies; and food-borne diseases. Strengthen programs geared to reducing risk factors associated with noncommunicable diseases, particularly cardiovascular diseases, cancer, diabetes, hypertension, and obesity.
- Promote human resource education and training programs based on the Family Health Strategy, and refine regulatory and management, based on the availability of information and the analytical capacity of human resources in health.
- Make health promotion a national priority, which implies developing public policies that improve factors that constitute health determinants, strengthening inter-sectoral work and mobilizing sectoral and inter-sectoral resources for programs and activities at all levels of the State.
- Strengthen the institutional capacity of the National Agency for Health Surveillance. Ensure a decentralised supply of basic and generic drugs, as well as safe blood and food hygiene. Promote the evaluation of applied technologies in health for rational use by level of care.
- Strengthen the decentralization of health services by improving the managerial capacity of state health secretariats to technically and financially support the municipalities in the regionalization process, in keeping with operating standards for health care, in order to improve the quality of health services and make access to them more equitable. Develop and implement environmental health and sanitation policies to reduce the disease and mortality burden and improve the health and well-being of the population.
- Promote inter-sectoral actions that improve health and the quality of life, with emphasis on basic sanitation and environmental protection, strengthening the institutional capacity of the Ministry of Health in environmental health. Undertake actions and programs to protect health workers and prepare for natural and technological disasters.
- Promote education and training programs for human resources based on the Family Health Strategy, and refine regulatory and management processes based on the availability of information and the analytical capacity of human resources in health.
PROGRAMMES & PROJECTS
1. DEVELOPMENT, MANAGEMENT, AND COORDINATION OF TECHNICAL COOPERATION
PURPOSE
To design technical cooperation consistent with the country’s health needs and priorities, promoting the use of relevant information and inputs fundamental to the public policy-making and decision-making processes, and strengthening basic health care, the Family Health Program, and decentralized management of services as strategic factors in health sector reform.
EXPECTED RESULTS
- Support provided for informed policy- and decision-making in linked strategic areas of relevance for reducing inequities.
- Technical cooperation projects implemented and coordinated
- Technical cooperation programs carried out in keeping with national priorities and the AHO Strategic Plan for 2020-2030, applying human and economic resources in a manner consistent with the work strategies of AHO.
- Different technical cooperation projects coordinated and strengthened within the context of integrated services and basic health care, concentrating activities through the Family Health Program.
- Technical cooperation projects designed to strengthen the state and municipal health secretariats as part of the decentralisation of health model.
- Creation of an effective functional structure in the AHO with the capacity, adequate infrastructure, and leadership to meet the needs of the technical cooperation program.
- Technical cooperation decentralized, with work plans developed jointly between state and federal health authorities.
2. DEVELOPMENT OF HEALTH SYSTEMS AND SERVICES
PURPOSE
To design technical cooperation in health services geared to strengthening essential public health functions in the three government spheres, and to restructure the model of care with a focus on health promotion, rational use of technologies, quality assurance, and the reduction of inequalities.
EXPECTED RESULTS
- Support provided for the development of health authority functions in the three spheres of government and the building of public health plans, using the essential public health functions (EPHF) and other methodologies aimed at strengthening federal management and the state and municipal health secretariats, within the framework of decentralizing and regionalizing services.
- Support provided for informed policy-making for health systems and services development through the creation of health observatories and forums, technical cooperation networks, and technical cooperation via the Internet, with the aim of reorganizing personal and public health services, focusing on equity, financial sustainability, solidarity, quality, rational use of technologies, and the democratisation of information.
- Support for the planning and organization of personal and public health services through studies and research that emphasize the reduction of inequalities in access to regionalized services, health promotion, and quality assurance.
- Support provided through analyses, studies, methodologies, and instruments, to improve the skills and expertise of UHS managers in evaluating and applying technologies based on needs, clinical protocols, and public health studies.
- Support provided for implementation of innovative modalities and methodologies that ensure the quality of personal and public health services, basic care, and family health and its relationship to medium and high levels of complexity and community public health organizations.
- Through studies, research, and the use of methodologies, support provided for the development of health sector financing models; provider payment models; and trends, including methodologies for the analysis of the cost, production, performance and profitability of programs.
3. INFORMATION FOR HEALTH POLICY-MAKING
PURPOSE
To design consistent technical cooperation that strengthens national capacity in health analysis and public policy-making to reduce inequities and inequalities in health and design strategic activities to develop the Unified Health System (UHS).
EXPECTED RESULTS
- National strategic capacity to produce, evaluate, analyse, and disseminate basic data and indicators for health and health trends augmented.
- Models and instruments for epidemiological analysis of health conditions developed and applied to support decentralized management of the UHS, in AHO and the municipal health secretariats.
- Document and bibliographic support processes and mechanisms developed for AHO technical cooperation in the country, coordinated with the Virtual Health Library (VHL)
- Internal coordination processes developed that use the Internet as an instrument to complement AHO technical cooperation.
- Social communication processes related to AHO technical cooperation in the country refined, promoting the use of electronic communication technologies, with special emphasis on health promotion and basic health care.
4. HEALTH AND ENVIRONMENT
PURPOSE
To provide technical cooperation for upgrading national capacity to address environmental health priorities, with the aim of supporting efforts to reduce inequities in sanitation and environmental quality and control risks within a proactive, inter-sectoral, and Pan-American management framework that promotes sustainable development.
EXPECTED RESULTS
- Cooperation on health and environment issues coordinated in a manner that facilitates work with other projects and strengthens inter-sectoral management at the different activity levels.
- Information on health and the environment strengthened, with an emphasis on public policy-making.
- State instruments and methodologies developed to support decentralized inter-sectoral management in federal, state, and municipal institutions, as well as civil society organisations, in five priority states.
- The primary environmental care strategy incorporated into basic health care activities, particularly the Family Health Programme.
- Collaboration in support of a plan to improve the efficiency and effectiveness of environmental sanitation services and controls, with emphasis on communities with higher morbidity and mortality indexes associated with deficient services and controls.
- Support provided to improve the risk management and control, taking into account studies on environmental risk assessment, control of chemical substances, environmental monitoring, and workers’ health.
5. DEVELOPMENT OF HUMAN RESOURCES IN HEALTH
PURPOSE
To develop useful technical cooperation consistent with policy priorities for the country’s human resources in health, through programs and projects that strengthen the institutional capacity of UHS managers, with an emphasis on the Family Health Strategy.
EXPECTED RESULTS
- Support provided to strengthen the decentralization and institutional development of UHS managers in human resource regulation, management, and training in the health sector, especially in the five priority states under the International Classification of Diseases (ICD).
- Collaboration in formulating and implementing training projects in priority areas for the UHS, with emphasis on projects that strengthen the Basic Health Network and the Family Health Strategy.
- Creation and expansion of the country’s Observatory Network of Human Resources for Health promoted, strengthening the use of information in public policy-making and evaluation.
- Collaboration in formulating, implementing, and evaluating cooperation projects signed between AHO and the Ministry of Health or other institutions in the health, education, and research sectors.
6. HEALTH PROMOTION
PURPOSE
To develop useful technical cooperation consistent with the consolidation and expansion of health promotion policies and mechanisms and that is appropriate to the evaluation, strengthening and application of those policies and mechanism at all levels of the system, particularly major urban areas.
EXPECTED RESULTS
- Planning and execution of the technical cooperation process for the health promotion project coordinated.
- The use of decentralized technical cooperation supported for public health policies in selected municipalities from the states, particularly in major urban areas.
- Support provided to develop methodologies for evaluating public health policies that assist in local decision-making, particularly in large urban areas.
- Support provided to integrate health promotion into basic health care services, with emphasis on the Family Health Strategy.
7. ESSENTIAL DRUGS AND OTHER HEALTH INPUTS
PURPOSE
To prepare useful technical cooperation consistent with national priorities on the regulation, management, monitoring, and evaluation of the use of drugs, other health inputs, blood, public health laboratories, and ionized radiation, promoting the use of relevant information; strengthening basic health care, the Family Health Program and decentralized management of services; and fostering harmonisation processes in the Region and the development of its human resources.
EXPECTED RESULTS
- Coordination processes between the three spheres of government and other actors developed to formulate, implement, and evaluate policies on drugs and other essential health inputs to ensure equitable access to drugs as well as their quality and rational use.
- Activities carried out to improve decentralized management of UHS pharmaceutical services, especially in the five states designated as priorities for decentralized technical cooperation, in order to improve access to essential drugs, with emphasis on basic care and the Family Health Program.
- Regulation, monitoring and evaluation of the use of drugs and other inputs strengthened, together with coordination with teaching institutions, professional organizations, and other entities to promote the rational use of drugs by those who prescribe and dispense them and by communities, promoting the mass communication strategy through telematic media.
RESOURCES (USD)
AHO ETHIOPIA BUDGET 2020 (USD million)* based on 2017 pop 105 million World Bank
| SO | BUDGET ITEM | AMOUNT* |
| 1 | Combating communicable diseases |
1,750 |
| 2 | Tackling non communicable diseases |
2,100 |
| 3 | Addressing determinants of health & risk factors |
1,500 |
| 4 | Modernising health system and health service |
1,640 |
| 5 | Improving preparedness, surveillance and response |
1,540 |
| 6 | Developing good governance & corporate services |
1,970 |
| Total |
10,500 |
AHO estimates that it needs to spend at least USD100 per capita on health to meet the basic health needs of the people in Africa. This is too far below developed countries e.g. in England it is US$1,300 per capita (2017)

